Research & Education
Defining Photomedicine
Photomedicine is an interdisciplinary branch of medicine that involves the study and application of light with respect to health and disease. Photomedicine may be related to the practice of various fields of medicine including dermatology, surgery, interventional radiology, optical diagnostics, cardiology, circadian rhythm sleep disorders and oncology. A branch of photomedicine is light therapy - the use of applicable volumes of light energy in specific infrared wavelengths to stimulate and energize sick or injured tissues and bring them back to full metabolic function. From: Lasers in Medicine, 2021
Primary Benefits of Photomedicine
Photomedicine (Laser Therapy) includes therapeutic applications of light for detecting and curing disease. Light is composed of packets of energy called photons. Therapeutic Light is defined as non-ionizing electromagnetic radiation between the wavelengths of about 200 nm to about 1200 nm. Light energy is capable of causing heating, mechanical effects and chemical reactions. The transfer of light energy through photon absorption can lead to many different beneficial consequences in photomedicine. Moreover, there are many new approaches for using light to see inside the body to detect and diagnose disease. Unlike pharmacological treatments that mask pain or only address the symptoms of disease, photomedicine treats underlying pathology to promote healing; meaning photomedicine treatments can be more effective than pharmacology, including no side effects and longer lasting benefits.
Photomedicine and Dose Effectiveness
Laser therapy dose effectiveness is dependent on a variety of patient tissue factors, all other variables being equal - i.e. wavelength(s), output power, etc.; for example, degenerative disc disease usually requires a large volume of high-output energy for effective tissue interactions, while oral cavity sores require only a small volume of low-output energy to successfully treat; effective treatment application for most other conditions lie somewhere in between. The reason for this is oral cavity sores exist in shallow, pigmented, moist, warm tissues with a plentiful blood supply, while injured discs are non-pigmented and protected by layers of densely complicated structural tissues without an independent blood supply.
Primary Response of Photomedicine
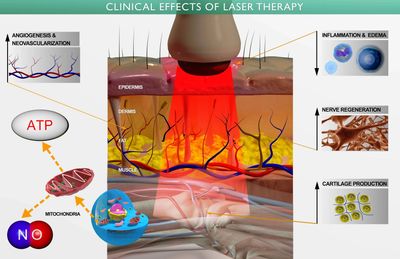
Primary response in photomedicine is elicited when photons emitted by the laser reach the mitochondria and cell membranes of underlying cells such as fibroblasts, where photonic energy is absorbed by chromophores and is converted to chemical kinetic energy within the cell. Chromophores absorb photons with wavelengths between 700 and 1200 nanometers (NIR, or near infra-red), with those in the 808nm and 980nm wavelengths being the deepest penetrating.
Secondary Responses
Secondary reactions lead to the amplification of the primary actions. A cascade of metabolic effects results in various physiological changes at the cellular level—such as changes in cell membrane permeability. Calcium is released from the mitochondria resulting in changes of intracellular calcium levels. This stimulates cell metabolism and the regulation of signaling pathways responsible for significant events required for tissue repair such as cell migration, RNA and DNA synthesis, cell mitosis, protein secretion, and cell proliferation.
Tertiary Responses
Additional responses are induced at a distance from the cells in which the secondary events occur. Energized (irradiated) cells communicate with each other and with nonirradiated cells through increased levels of cytokines or growth factors, along with correlating electromagnetic energy field interactions. This intercellular communication on the cellular biochemical and electromagnetic energy field levels results in an increase in (ATP) Adenosine Triphosphate production, enhanced immune response with the increased activation of T-lymphocytes, macrophages, and number of mast cells, an increase in the synthesis of endorphins, and a decrease in bradykinin results in pain relief, and a general increase in the energy levels of targeted tissues, as well as additional beneficial interactions. While tertiary effects can be least predictable because they rely on intercellular interactions and vary according to tissue factor variables, they can be most profound and have a major effect on beneficial targeted tissue interactions.
Copyright © 2024 Advanced Medical Distributors, LLC - All Rights Reserved.
This website uses cookies.
We use cookies to analyze website traffic and optimize your website experience. By accepting our use of cookies, your data will be aggregated with all other user data.